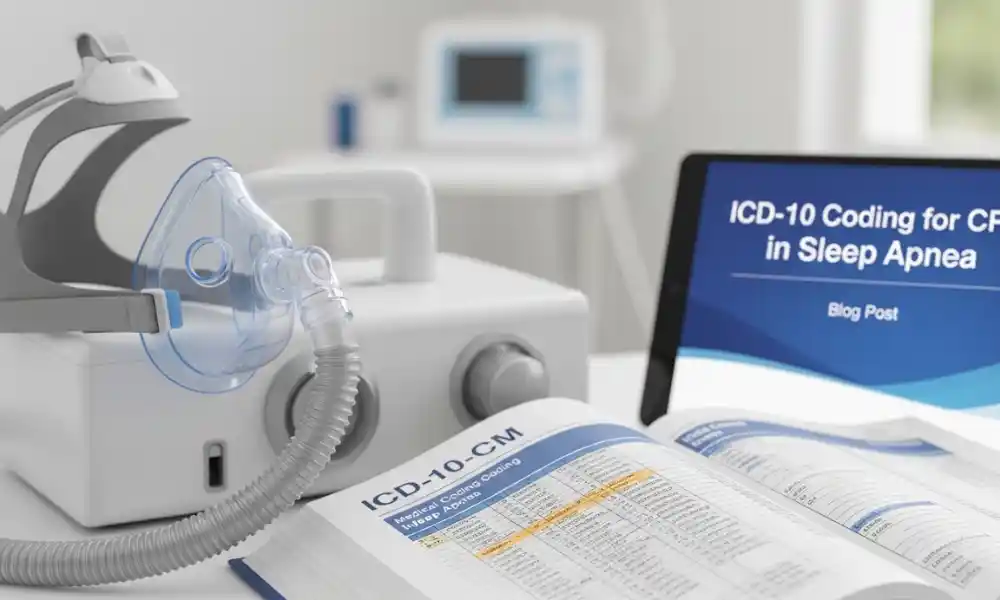
Sleep apnea is one of the most common sleep disorders affecting millions of adults worldwide. Continuous Positive Airway Pressure (CPAP) therapy is considered the gold-standard treatment for obstructive sleep apnea (OSA). However, from a medical billing perspective, prescribing a CPAP machine requires accurate diagnosis coding, documentation, and compliance with payer requirements.
Healthcare providers, sleep clinics, and medical billers must understand the correct ICD-10 coding for CPAP therapy in sleep apnea to ensure proper reimbursement and avoid claim denials.
This guide explains everything you need to know about CPAP ICD-10 coding for CPAP therapy, including diagnosis codes, billing requirements, documentation guidelines, and common coding mistakes.
Understanding Sleep Apnea and CPAP Therapy
What Is Sleep Apnea?
Sleep apnea is a sleep disorder characterized by repeated interruptions in breathing during sleep. These interruptions can occur dozens or even hundreds of times per night.
The condition leads to symptoms such as:
- Loud snoring
- Daytime fatigue
- Morning headaches
- Difficulty concentrating
- Interrupted sleep patterns
If untreated, sleep apnea can increase the risk of serious health conditions such as heart disease, hypertension, diabetes, and stroke.
What Is CPAP Therapy?
CPAP stands for Continuous Positive Airway Pressure. It is a medical device that delivers steady air pressure through a mask to keep the airway open during sleep.
CPAP therapy helps:
- Prevent airway collapse
- Improve breathing during sleep
- Reduce daytime fatigue
- Improve oxygen levels
Because CPAP devices are classified as Durable Medical Equipment (DME), insurance companies require proper documentation and diagnosis coding before approving coverage.
ICD-10 Codes for Sleep Apnea Used With CPAP
Accurate ICD-10 coding is essential for medical billing related to CPAP therapy.
Primary ICD-10 Code for CPAP Therapy

G47.33 – Obstructive Sleep Apnea (OSA)
This is the most commonly used cpap ICD-10 code for CPAP billing.
It applies when a patient is diagnosed with obstructive sleep apnea confirmed through a sleep study.
Most insurance providers require this diagnosis code before approving CPAP therapy.
Other ICD-10 Codes for Sleep Apnea
G47.30 – Sleep Apnea, Unspecified
Used when the type of sleep apnea is not documented. However, many insurers reject claims using this code for CPAP therapy.
G47.31 – Central Sleep Apnea
This condition occurs when the brain fails to send proper signals to breathing muscles.
G47.37 – Central Sleep Apnea in Conditions Classified Elsewhere
Used when central sleep apnea is caused by another underlying medical condition.
G47.39 – Other Sleep Apnea
Used for rare or mixed sleep apnea types.
Choosing the correct ICD-10 code is critical because it determines whether the CPAP device will be approved for reimbursement.
ICD-10 Code for CPAP Dependence
In some cases, providers may document long-term dependence on CPAP therapy.
Z99.89 – Dependence on Other Enabling Machines and Devices
This code may be used when documentation shows that the patient relies on CPAP therapy for breathing support.
However, it should not replace the primary diagnosis code for sleep apnea.
HCPCS Codes for CPAP Equipment
While ICD-10 codes describe the diagnosis, HCPCS codes represent the medical equipment used for treatment.
Common CPAP-related HCPCS codes include:
| HCPCS Code | Description |
|---|---|
| E0601 | CPAP device |
| A7030 | Full face mask |
| A7034 | Nasal mask |
| A7035 | CPAP headgear |
| A7037 | CPAP tubing |
| A7038 | CPAP filter |
Medical billing claims must include both HCPCS codes and the correct ICD-10 diagnosis code.
CPT Codes Associated With CPAP Therapy
Sleep apnea diagnosis often requires diagnostic procedures before CPAP therapy is prescribed.
Common CPT codes include:
| CPT Code | Description |
|---|---|
| 95810 | Polysomnography sleep study |
| 95811 | Sleep study with CPAP titration |
| 94660 | CPAP initiation and management |
These procedures help confirm the diagnosis and determine the appropriate CPAP pressure settings.
Documentation Requirements for CPAP Billing
Insurance providers require detailed documentation before approving CPAP therapy.
Key documentation elements include:
Sleep Study Results
A sleep study (polysomnography) must confirm sleep apnea diagnosis.
Apnea Hypopnea Index (AHI)
AHI measures the severity of sleep apnea.
Typical criteria include:
- AHI ≥ 15 events per hour
- AHI ≥ 5 with symptoms such as fatigue or hypertension
Clinical Symptoms
Documentation should include symptoms such as:
- Daytime sleepiness
- Loud snoring
- Observed breathing pauses
- Morning headaches
Physician Recommendation
The provider must clearly document the need for CPAP therapy.
Proper documentation ensures that claims meet payer medical necessity requirements.
Medicare Requirements for CPAP Coverage
Medicare and many private insurers follow strict guidelines for CPAP coverage.
Patients must have:
- Confirmed diagnosis of obstructive sleep apnea
- A qualifying sleep study
- Physician prescription for CPAP therapy
- Documentation of symptoms and severity
Failure to meet these requirements may result in claim denials.
CPAP Compliance Monitoring
Many insurers require proof that patients are actually using their CPAP devices.
Typical compliance standards include:
- CPAP usage at least 4 hours per night
- Usage on 70% of nights
Providers must document patient adherence through CPAP machine data reports.
Failure to demonstrate compliance may cause insurers to stop coverage.
Common ICD-10 Coding Mistakes in CPAP Billing
Medical billing errors can delay CPAP treatment and reimbursement.
Using Unspecified Diagnosis Codes
Claims using G47.30 (unspecified sleep apnea) are often denied.
Missing Sleep Study Documentation
Insurance companies require sleep study confirmation.
Incorrect Diagnosis Coding
Coding central sleep apnea instead of obstructive sleep apnea can cause claim rejection.
Missing Equipment Codes
CPAP claims must include HCPCS codes for equipment.
Avoiding these mistakes improves claim approval rates.
Best Practices for Accurate CPAP Coding
Healthcare providers and medical billers should follow these best practices:
Verify Diagnosis
Always confirm the specific type of sleep apnea.
Use Specific ICD-10 Codes
Avoid unspecified diagnosis codes whenever possible.
Maintain Complete Documentation
Include sleep study results and symptom documentation.
Link Diagnosis and Equipment Codes
Ensure ICD-10 diagnosis codes match HCPCS equipment codes.
Perform Billing Audits
Regular audits help detect coding errors and reduce denials.
Role of Medical Billing Companies in Sleep Apnea Coding
Because sleep apnea billing involves multiple coding systems, many healthcare providers outsource billing to specialized medical billing companies.
Benefits include:
- Reduced claim denials
- Faster reimbursement
- Accurate coding compliance
- Better revenue cycle management
Professional billing services help practices navigate complex payer rules.
Frequently Asked Questions
What is the ICD-10 code for CPAP therapy?
The most common ICD-10 code used with CPAP therapy is G47.33 for obstructive sleep apnea.
What is the ICD-10 code for CPAP use?
There is no specific ICD-10 code for CPAP use; it is typically reported with G47.33 (obstructive sleep apnea) and, if applicable, Z99.89 (dependence on medical devices).
What diagnosis for CPAP?
The primary diagnosis for CPAP therapy is G47.33 (obstructive sleep apnea).
When to use Z99-89?
What is the minimum AHI required for CPAP therapy?
Typically:
- AHI ≥ 15, or
- AHI ≥ 5 with symptoms or comorbid conditions.
Final Thoughts
ICD-10 coding for CPAP therapy in sleep apnea requires careful attention to diagnosis accuracy, documentation, and insurance requirements. Proper coding ensures that patients receive timely treatment while healthcare providers receive appropriate reimbursement.
Key takeaways include:
- Use G47.33 for obstructive sleep apnea whenever appropriate
- Include supporting documentation such as sleep study results
- Link diagnosis codes with correct HCPCS equipment codes
- Monitor patient compliance for continued coverage
With accurate coding and documentation, healthcare providers can reduce claim denials, improve reimbursement rates, and ensure that patients receive effective treatment for sleep apnea.
For healthcare providers looking to simplify the process and avoid costly errors, Billing Care offers expert medical billing services tailored to CPAP and sleep apnea coding, helping you stay compliant while maximizing revenue.